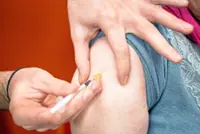
I believe that there are lots of people who just need to be given more information and reassurance that whatever vaccines that are approved for use in Malaysia are safe and effective, based on clinical trials involving lots of volunteers, whether from here or elsewhere.
When it comes to evaluating new treatments, clinical trials remain the “gold standard” as they are actually tested on humans, rather than in the lab or via computer modelling. By this, it means testing is done on sufficiently large cohorts of people, and not just in a small group, in order to arrive at conclusive findings. On a global scale, the Comirnaty and mRNA-1273 vaccines from Pfizer-BioNTech and Moderna TX respectively, both based on mRNA technology, have undergone extensive clinical trials (outside Malaysia) to be where they are now.
Already a subscriber? Log in
The Star 6.6 DEAL: 35% OFF Digital Access
Cancel anytime. Ad-free. Unlimited access with perks.