In 2022, the National Health and Morbidity Survey (Maternal and Child Health) reported that 46.5% of children aged zero to five years old have anaemia, or low iron levels.
It was higher than what the World Health Organisation (WHO) estimated for Malaysia (24.6%). It was also more than the global average of 40%.
Over the years, senior consultant paediatric endocrinologist Prof Dr Muhammad Yazid Jalaludin has been vocal about this issue, emphasising iron screening and a better diet.
An “unseen” condition, iron-deficiency anaemia (IDA) in kids is often uninvestigated. While parents of young children know about developmental milestones or early intervention, iron levels – which may affect learning, cognition and physical growth – are rarely given much thought.
“Some symptoms such as paleness, weakness, loss of appetite, fatigue and lethargy are non-specific and usually appear only at more severe stages of anaemia. Many parents do not realise their children are experiencing anaemia because access to IDA screening is limited,” he adds.
Failing to address this issue, he says, may result in a younger generation that has its intelligent quotient (IQ), growth and immunity compromised.
He says research shows IDA poses irreversible cognitive and developmental harm.
“Even mild iron deficiency can impact a child’s growth and have consequences on their brain development and future learning abilities,” he says.
“Studies have shown that iron deficiency may see a child’s IQ drop by 13%. Brain synapses that connect neurons need iron and chronically low haemoglobin levels lead to poor growth,” he adds.
“Iron deficiency also affects the body’s ability to produce adequate immune response, making the person more susceptible to infections.”
On top of that, children with IDA often experience fatigue, weakness and lack of focus.
“These symptoms can make it difficult for them to participate in school, play and do other daily activities,” he says.
An unseen problem
Because the symptoms of IDA are not obvious, screening for the condition and efforts on educating parents about the importance of iron-rich food aren’t widespread.
Dr Muhammad Yazid says everyone is born with an iron store but at six months old, when complementary feeding starts, this storage reduces if food given isn’t iron-rich.
“Most parents puree fruits and vegetables, like pumpkin and carrot to feed their kids. If this diet continues and parents don’t include food rich in iron, that iron store will keep depleting,” he says.
“At 12 months old, food given should include animal protein which is a source of heme iron, a type more readily absorbed by the body,” he says.
The dean of the Faculty of Medicine, Universiti Malaya also says a study carried out by Universiti Malaya Medical Centre (UMMC) found that iron store starts reducing at three months old.
This, he says, underlines the importance of keeping mothers very healthy with adequate iron intake throughout breastfeeding so their young offspring will get enough iron.
“Of course, creating a good ‘iron store’ begins in-utero. But the supplementation for mothers should continue after they give birth, for as long as they breastfeed, for their children to benefit from it,” he adds.

Feeding kids better
As kids grow, Dr Muhammad Yazid says parents need to feed them differently.
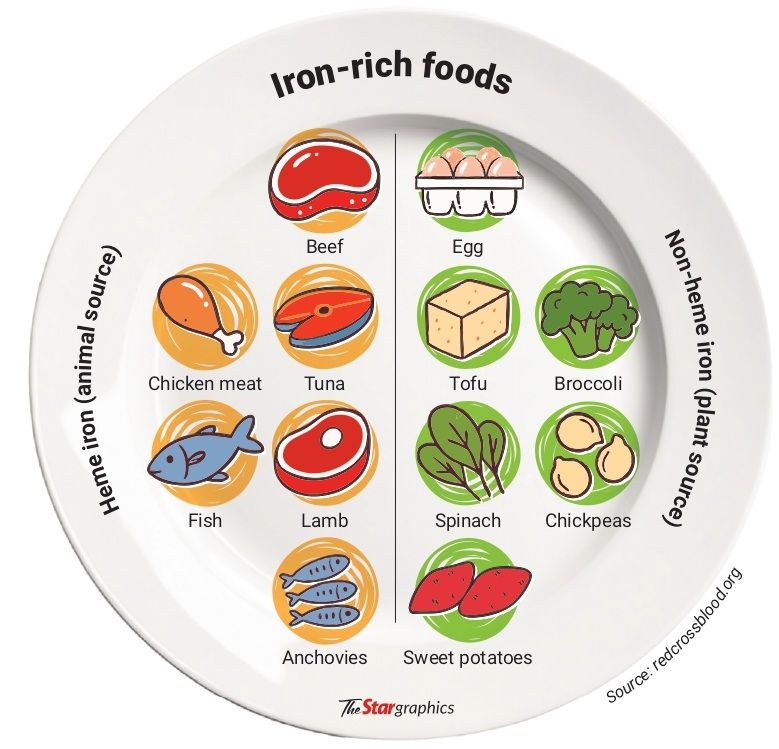
“Give them iron-rich foods such as beef, lamb, liver, chicken and anchovies. Plant sources (non-heme iron) include tofu, eggs, kangkung, spinach and chick peas,” he says.
“Parents can also combine iron-rich food with vitamin C food like citrus fruits, guava and papaya, which will help boost the mineral’s absorption,” he says.
Dr Muhammad Yazid admits the rising cost of living affects household food security and nutrition quality, especially among vulnerable groups.
“When staple foods and nutrient-rich items (like meat and leafy greens) become less affordable, families may shift to cheaper, less nutritious diets. This shift increases the risk of micronutrient deficiencies, including IDA,” he says.
However, higher income does not always mean better nutrition.
“Some wealthier families still choose processed and convenient foods that are low in iron. Time is also essential for working parents, so some opt for quicker food to feed their children, which can be less nutritious,” he adds.
Lower-income families can still provide healthy, balanced meals if they are aware of affordable, iron-rich options like anchovies, chicken, tofu, eggs and leafy greens.
“The real difference is parental awareness of how crucial iron is for brain development, immunity and growth,” he says.
Nutrition education across all income levels is critical and mandatory IDA screening as part of child health programmes would help ensure no child is overlooked.
On top of that, current collaborations with ministries and partners are already working to embed screening and expand support for vulnerable families.
“Small, consistent changes in daily meals can prevent IDA, and screening remains a key step in catching it early,” he concludes.





