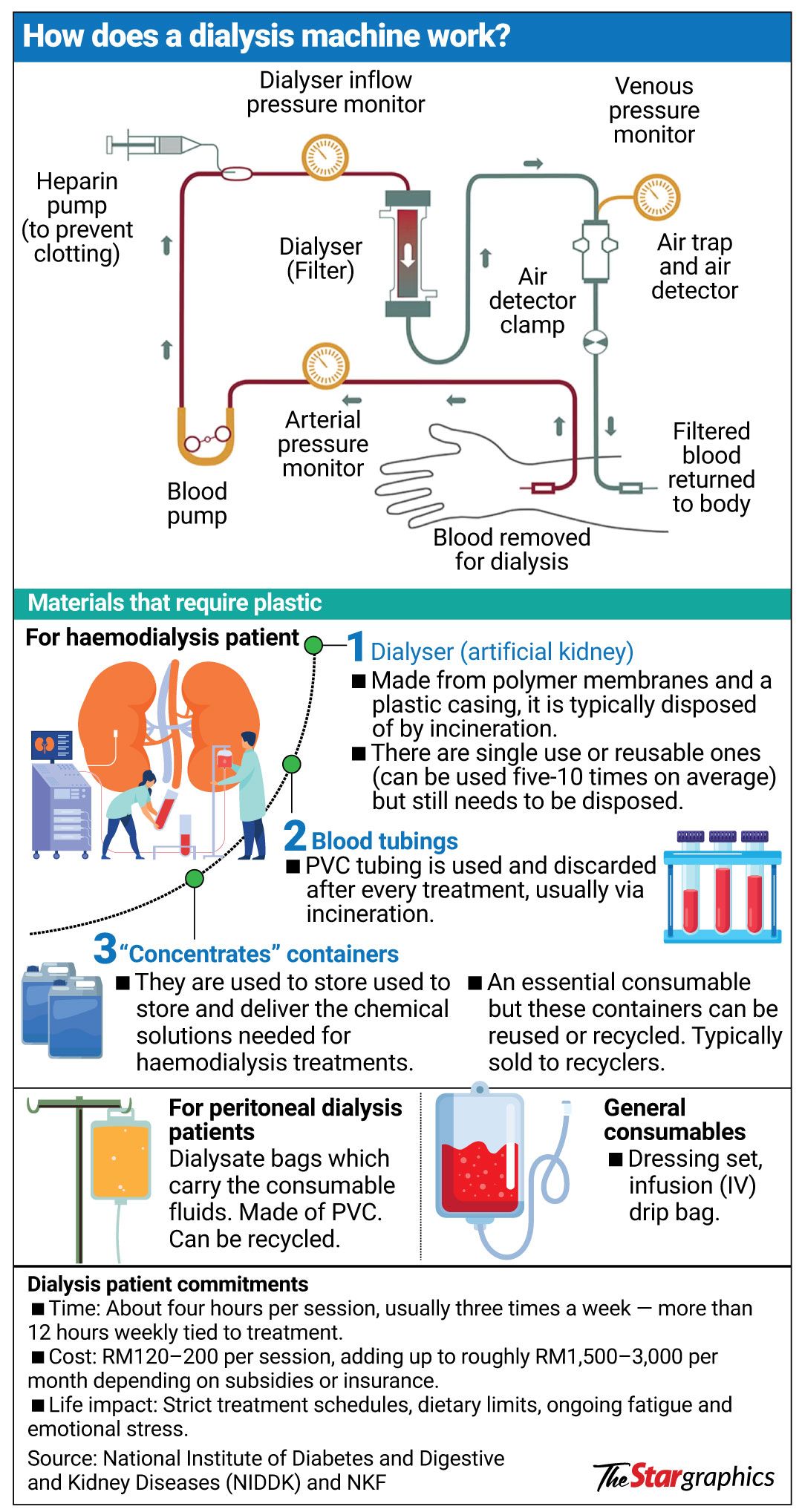
Greener solutions needed to protect environment
PETALING JAYA: Dialysis has an environmental cost, but this cannot compromise patient care.
The challenge is to make dialysis greener without reducing access or safety, says the National Kidney Foundation (NKF).
Its chief executive officer Choo Kok Ming said dialysis treatments such as haemodialysis and peritoneal dialysis are resource-intensive medical therapies, relying on disposable materials and consuming large amounts of water and energy.
ALSO READ: Patients struggle with ‘draining’ reality of treatments
However, he noted that peritoneal dialysis has a relatively lower carbon impact compared to in-centre haemodialysis treatment.
He was referring to the Health Ministry, which recently said haemodialysis in Malaysia consumes approximately 250 to 500 litres of water per session, totalling over two billion litres annually for roughly 50,000 patients.
“The life cycle analysis (LCA) for dialysis treatment indicates a high carbon footprint,” said Choo.
“This is mainly due to the transportation of patients, staff and suppliers, the use of electricity and water, and packaging materials and consumables for treatment.”
LCA is a method used to measure the total environmental impact of something across its entire life cycle.
Dialysis is required for chronic kidney disease, majority of which is driven by metabolic conditions like hypertension and diabetes.
In 2024, about 21% of Malaysian population are diabetics, or one in every five people, according to data from the World Bank.
When asked what dialysis centres could do to save water without affecting patient safety, Choo said centres should choose more efficient water treatment systems that produce less reject water.
He added that routine maintenance of treatment systems, water pipes and machines is also important to detect leaks early.
“All haemodialysis treatments require the use of ultra-pure water so that it is free from toxins, heavy metals, bacteria and other contaminants that could enter the bloodstream and cause serious health complications.
“The water is purified with a reverse osmosis (RO) water treatment system whereby there is ‘reject water’ that can be used for other non-clinical means like cleaning.
“Centres should also review dialysate flow rates to reduce water use per treatment in line with evidence-based and patients’ clinical needs to ensure it does not affect dialysis adequacy,” he said.
On plastics, he said suppliers are choosing lighter or non-PVC plastics for manufactured consumables, but pricing remains a key consideration.
He said most centres already reuse plastic containers or sell them to be reused, including recycling unused ones, but stressed that proper waste segregation practices are important.
Choo noted that peritoneal dialysis (PD) cases, which require bulk deliveries of fluid bags, can be optimised by balancing load and delivery frequency, especially in more rural areas.
He added that NKF has also focused on reducing dependence on dialysis treatment by promoting preventive healthcare practices and kidney transplantation, as well as green nephrology.
“Government should also set policy frameworks and accompanying incentives for water efficiency, renewable energy use and support capital investments for such adoptions.
“Centre design matters too. Larger centres that combine all types of kidney care, including preventive medicine, and are properly designed to optimise water and energy use will be more environmentally friendly and sustainable in the long run,” he said.
For now, Choo said centres should first eliminate waste and inefficiency and prioritise changes that do not compromise care.
“Green dialysis is not about choosing between life-sustaining treatments for patients and the planet. It is about reducing avoidable damage to the environment while delivering high-quality, life-saving treatment,” he added.
Meanwhile, Association of Water and Energy Research Malaysia (AWER) president Piarapakaran S. suggested more detailed monitoring of water use across separate operations.
“The industry can find a way forward to minimise water use without jeopardising patient safety or efforts to prevent infection or contamination. We can look into being more sustainable, but not at the risk of compromising safety and patients’ well-being.
“At the end of the day, the maturity of technology is key to addressing specific issues in the healthcare sector. Even operating theatres have very specific requirements to ensure safe procedures,” said Piarapakaran, who is also the Centre for Water and Energy Sustainability chief executive officer.
He added there was a need for a step-by-step approach assisted by technology and sound data before making any rapid changes, with healthcare professionals overriding the changes if they see risk.