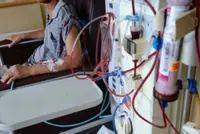
We are born with two kidneys and although we only need one to survive, chronic kidney disease (CKD) is a common ailment.
According to the Global Burden of Disease 2015 study, it is estimated that the 1.2 million deaths, 19 million disability-adjusted life-years and 18 million years of life lost from cardiovascular diseases are directly attributable to reduced glomerular filtration rates (GFR).
Already a subscriber? Log in
Get 20% OFF The Star Digital Access
Cancel anytime. Ad-free. Unlimited access with perks.